Featured Course
Dialysis Access Graft Evaluation
This course is designed to provide a detailed evaluation of dialysis access grafts, fistulas, and the mapping involved prior to surgery.
VIEW TRAINING COURSE
Case Study Details
50 year old African American female.
Swollen and painful left upper arm. Left upper arm hemodialysis access AVF with palpable thrill. End-stage renal disease secondary to lupus nephritis; history of mitral valve repair; on anticoagulation medication for atrial fibrillation.
Left upper extremity venous Doppler for evaluation for deep venous thrombosis.
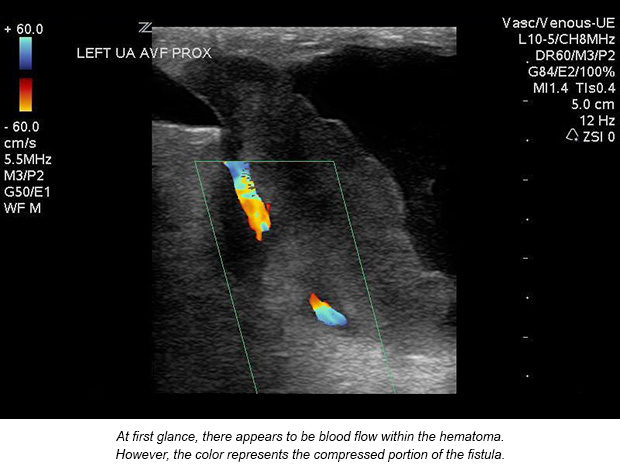
The exam was performed at the patient’s bedside seven days post-op for a hemodialysis access AVF. No evidence of deep or superficial venous thrombosis was found. A 7.2 cm mostly solid avascular mass was identified and appeared to be compressing the fistula.
A thorough investigation of the mass noting size, location, vascularity, and echogenicity is critical. A thrombosed pseudoaneurysm was considered as a differential diagnosis.
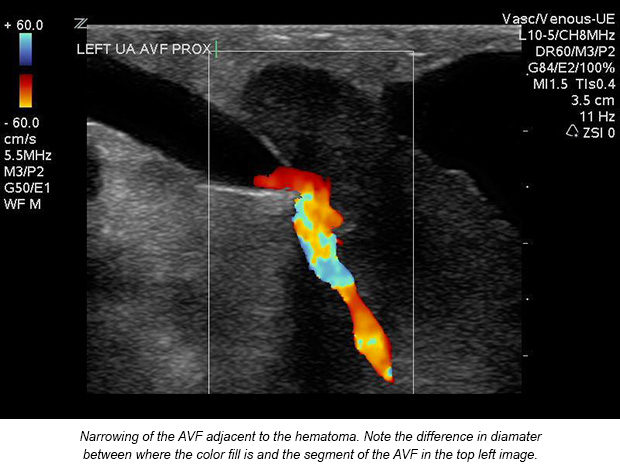
The area was concluded to be an infected hematoma. A follow-up ultrasound five months later showed that the hematoma naturally resolved; however, the damage to the new fistula was too severe to regain a proper diameter. The patient is being dialyzed via Perm-a-Cath and is scheduled for angioplasty to attempt to dilate the fistula. She has stated that a family member has come forward and offered a kidney for transplant.
Tell Us Your Story
We want to hear how you are using Ultrasound to improve patient care. Email Us Your Story